 While alkaline (battery) injuries are usually deeper and worse than acid injuries, it is because the alkali sets up a type of necrosis called liquefactive necrosis. Acids cause coagulative necrosis. Alkaline ingestions cause tissue injury by liquefactive necrosis, a process that involves saponification of fats and solubilization of proteins. Cell death occurs from emulsification and disruption of cellular membranes. The hydroxide ion of the alkaline agent reacts with tissue collagen and causes it to swell and shorten. Small vessel thrombosis and heat production occurs.
While alkaline (battery) injuries are usually deeper and worse than acid injuries, it is because the alkali sets up a type of necrosis called liquefactive necrosis. Acids cause coagulative necrosis. Alkaline ingestions cause tissue injury by liquefactive necrosis, a process that involves saponification of fats and solubilization of proteins. Cell death occurs from emulsification and disruption of cellular membranes. The hydroxide ion of the alkaline agent reacts with tissue collagen and causes it to swell and shorten. Small vessel thrombosis and heat production occurs.
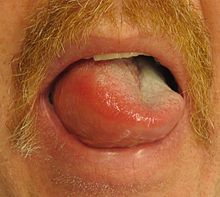
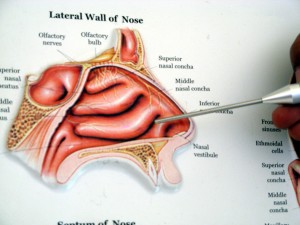
Severe injury occurs rapidly after alkaline ingestion, within minutes of contact. The most severely injured tissues are those that first contact the alkali, which is the squamous epithelial cells of the oropharynx, hypopharynx, and esophagus. The esophagus is the most commonly involved organ with the stomach much less frequently involved after alkaline ingestions. Tissue edema occurs immediately, may persist for 48 hours, and may eventually progress sufficiently to create airway obstruction. Over time, if the injury was severe enough, granulation tissue starts to replace necrotic tissue.
Over the next 2-4 weeks, any scar tissue formed initially remodels and may thicken and contract enough to form strictures. The likelihood of stricture formation primarily depends upon burn depth. Superficial burns result in strictures in fewer than 1% of cases, whereas full-thickness burns result in strictures in nearly 100% of cases. The most severe burns also may be associated with esophageal perforation.
Acid ingestions cause tissue injury by coagulation necrosis, which causes desiccation or denaturation of superficial tissue proteins, often resulting in the formation of an eschar or coagulum. This eschar may protect the underlying tissue from further damage. Unlike alkali ingestions, the stomach is the most commonly involved organ following an acid ingestion. This may due to some natural protection of the esophageal squamous epithelium. Small bowel exposure also occurs in about 20% of cases. Emesis may be induced by pyloric and antral spasm.
The eschar sloughs in 3-4 days and granulation tissue fills the defect. Perforation may occur at this time. A gastric outlet obstruction may develop as the scar tissue contracts over a 2- to 4-week period. Acute complications include gastric and intestinal perforation and upper gastrointestinal hemorrhage.



![delphian node[6]](http://www.midwestsinus.com/wp-content/uploads/2014/01/delphian-node6.png)